CASA Website > Avmed > Guidelines > Hyperglycaemia - Initial Assessment

Hyperglycaemia - Initial Assessment
Feedback
If you find any errors or omissions in these Guidelines, or feel that something in them needs to change, write to:
DameClinGuide.feedback@casa.gov.au
Please include details of the page on which you wish to provide feedback.
Thank you for your assistance in ensuring that these Guidelines are up to date and correct.
Search again
Indication
- Test as per DAME Reference Chart
- Fasting glucose 5.5mmol/L or more
- See below for action on HbA1c 6.5% [48mmol/mol] or over
Procedural requirements
- 75g glucose tolerance test following overnight fast
Interpretation
- HbA1c 6.5% [48mmol/mol] or over: assess as Diabetic
- 2hr glucose >11mmol OR Two fasting glucose readings > 7mmol: assess as Diabetic
- 2hr glucose between 7.8 and 11: assess as Impaired Glucose Tolerance (IGT)
- 2hr glucose less than 7.8mmol and fasting glucose >6mmol: assess as Impaired Fasting Glucose (IFG)
- ROLE of GTT and HbA1c: HbA1c levels have been validated in the diagnosis of diabetes. They have not been adequately validated in the estimation of cardiovascular disease risk, and cannot determine IFG and IGT, where elevated CVD risk also needs to be considered. For this reason, GTT remains the risk stratification tool where there is non-diabetic hyperglycaemia.
Further Actions
- Diabetes require workup as per schedule:
- Impaired Glucose Tolerance (IGT)
- Impaired Fasting Glucose (IFG)
Pilot Information
There is a strong link between abnormalities of glucose metabolism, heart disease and strokes. This includes both diabetes and “pre-diabetes”.
The consequences of heart attacks and strokes are potentially serious.
In addition, abnormal glucose levels can affect many of the body systems such as eyes, kidneys and nerves.
There are well proven ways of managing these risks once they are identified, and so accurate diagnosis is important.
References
Hyperglycaemia - Initial Assessment flowchart
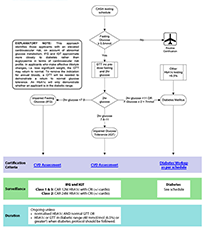
Select the image for a detailed view.
A text version of the Hyperglycaemia - Initial Assessment flowchart is also available.
Disclaimer
The Clinical Practice Guideline is provided by way of guidance only and subject to the Clinical practice guidelines disclaimer

